Rural Health Has a Last-Mile Data Problem. FHIR Is Part of the Answer.

Health systems have made real progress on interoperability. But outside clinical walls, rural care teams, community paramedics, and family caregivers are still stitching records together by hand. Primary Record co-founder Jean Ross, RN, on the last-mile data problem in care coordination, and what FHIR can and can’t yet solve.
Why Do We Build Medical Care Pathways But Not Social Ones?

We’ve spent decades building clinical pathways for heart failure: the drugs, the testing intervals, the escalation triggers. But the pathway stops at the hospital door. The community paramedic, the area agency on aging, the community health worker, they’re doing the work that keeps patients out of the ER, and none of them are in the same system, reliably funded, or connected to each other. It’s time to build the care pathway that starts when the patient goes home.
There Is No Official “HIPAA Compliance Logo.” Here’s What to Look for Instead.

Many families think they need to look for a HIPAA compliance logo when choosing a health app, but no official logo actually exists. Learn what certifications really matter and how to choose tools that truly protect your health information.
The Portal Paradox: What Rural Health Programs Must Know Before Investing in Interoperability

Rural health committees can learn from big systems’ expensive interoperability mistakes without inheriting problems they lack the resources to fix. Learn how to evaluate vendors and protect your investment.
Interoperability Isn’t a Technology Problem Anymore. It’s a Trust Problem.
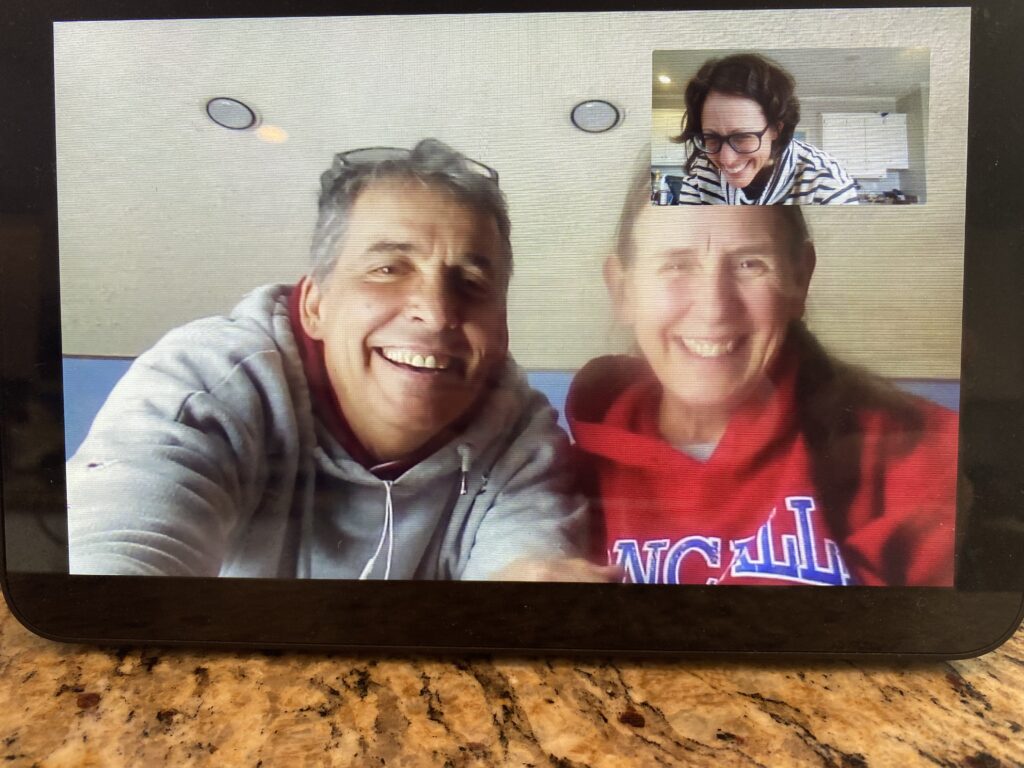
For years, healthcare data sharing has been treated as a technology problem. But faster software and better standards haven’t solved the real barrier: trust. As information moves across hospitals, communities, and homes, the question isn’t whether we can share data, it’s whether we’ve built the trust systems needed to do it safely and well.
Who Will Make My Medical Decisions? Childfree Trust’s Care Planning Model

The launch of Childfree Trust signals a shift the advocacy and life care planning community has long been preparing for: planning isn’t just about naming someone, it’s about equipping them. This article examines the hidden labor behind POA and fiduciary roles, and why shared, living information is essential to confident, compassionate care.
Why ‘Just Give Me Your Login’ Puts Caregivers and Advocates at Risk
Many patient advocates and caregivers rely on shared logins or HIPAA authorizations to access medical records, often without realizing the legal and ethical risks. This article explains the critical difference between HIPAA Authorization and the HIPAA Right of Access, and what safer, patient-directed access really looks like.
Patient-Directed Interoperability: Delivering the Last Mile of Health Data Into Homes and Communities

Interoperability breaks where care actually happens: at the kitchen table and across community care teams. This article explores why patient-directed interoperability and FHIR are essential to rural health transformation and last-mile care coordination.
The ROI of Patient Access APIs That No Health Plan Is Measuring…Yet

Health plans have spent millions building Patient Access APIs, but few understand what actually happens once the data reaches members and caregivers. Real ROI doesn’t come from FHIR servers or compliance checkboxes. It comes from the last mile of interoperability: when families can finally see, understand, and use their own data to prevent crises, close care gaps, and make better decisions at key moments of care.
