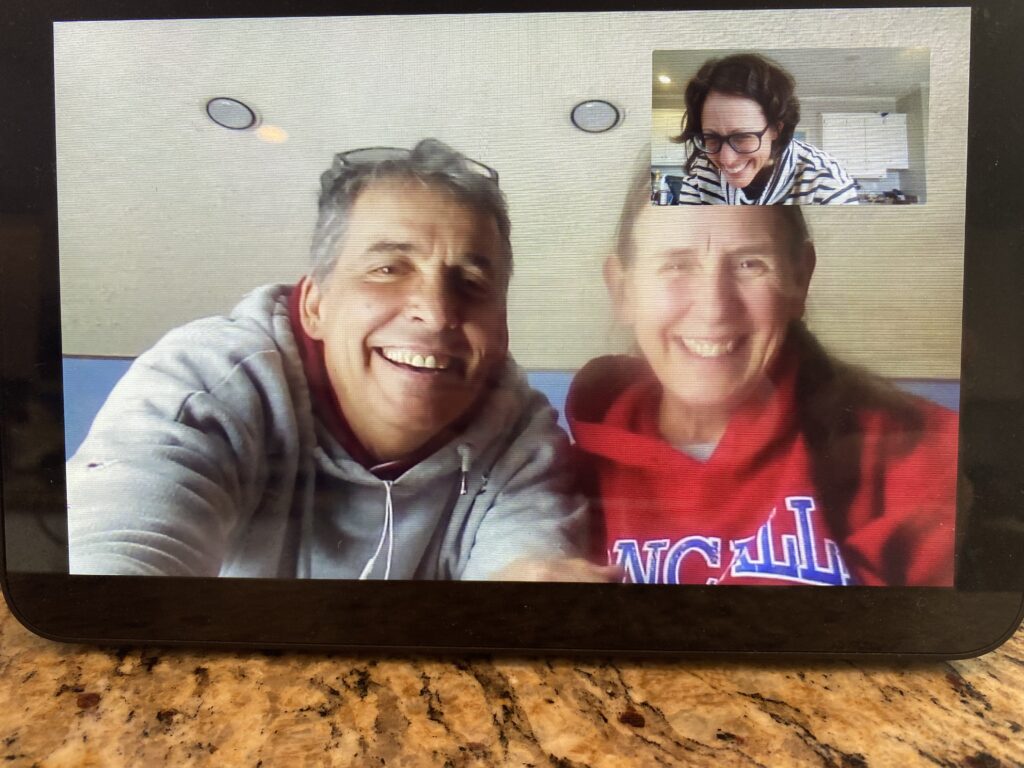
Last week, a nurse proudly told me, “We have a centralized portal that we’re happy with.”
I believed her. She should be happy with it. It probably works beautifully…for her hospital.
But here’s the question I wish I’d asked: “How many portals does Mr. Rodriguez have passwords for right now?”
Rural health programs pursuing the same electronic health record (EHR) systems as large health systems need to understand something: buying the same EHR doesn’t mean all your problems go away.
This portal burden is the hidden cost of health technology investment, one that big health systems created with unlimited IT budgets and staff, and that rural communities will inherit without those same resources. The question isn’t whether to invest in interoperability. It’s whether you’ll repeat urban America’s expensive mistakes or learn from them.
The View from 30,000 Feet
From inside your organization, staff see their source of truth. Clean. Organized. Everything a patient needs from them is in one place.
From a patient’s kitchen table, it looks different:
- LabCorp portal for the pre-op bloodwork
- Cardiologist’s office portal (different health system)
- Primary care portal (another system)
- Home health agency portal (if they’re lucky enough to get login credentials)
- Your hospital’s portal
- Imaging center portal for the follow-up CT
Six portals. Six usernames. Six passwords. Six different interfaces.
And we wonder why patients and caregivers are hard to reach and engage.
From the organization’s point of view, the box is checked: we provided access.
From the family’s point of view, the work has just begun.
And that gap matters.
- It affects readmissions, because information doesn’t move with the patient
- It affects staff burnout, because nurses and care managers re-collect data that already exists
- It affects patient engagement, because people disengage when systems don’t match how care actually happens across settings
This isn’t because anyone did anything wrong.
It’s because portals were built for institutional access, not for longitudinal, shared, community-involved care. And for rural health programs, every technology investment must work harder, across more miles, with fewer staff, and often with less vendor support than urban health systems receive.
And transitions are where outcomes are won or lost.
Three Questions We’re Not Asking (But Should Be)
1. “Can your patients actually access what you’re sharing?”
Your 68-year-old heart failure patient gets discharged on a Friday. He needs to share his new medication list with his home health nurse on Monday and his new cardiologist on Thursday.
Does he know how to download it from your portal? Does he remember the password he created while dizzy from having his blood pressure meds adjusted? Can his daughter access it to help? Or does he just bring in that crumpled paper from the kitchen table, while the cardiologist’s office faxes you for the information?
2. “What happens to care coordination when information lives in silos?”
Your physical therapist makes a crucial observation about mobility decline. It goes in your portal notes. Meanwhile, the home care nurse, working from a different agency, documents increased fall risk in their system. The primary care doctor, preparing for tomorrow’s appointment, sees neither note.
Three professionals. Three systems. One patient is falling through the gaps.
3. “Are we accidentally making our own jobs harder?”
When patients can’t access or share information across portals, who gets the phone calls? Who fields the fax requests? Who manually re-enters information that already exists somewhere else?
That’s not a technology problem. That’s a retention problem disguised as a workflow issue.
The Certification Question Nobody’s Talking About
Here’s something many frontline teams don’t realize, and something critical for rural health technology investment decisions:
Your electronic health record (EHR) may be certified health IT, but that doesn’t mean patients or community partners can actually use the data the way federal policy intended.
The real questions are:
Is your organization participating in health information exchange (HIE) beyond your own network? If not, your “interoperable” system may only talk to hospitals like you, not hospitals in another state, home health, EMS, specialists across town, or community organizations.
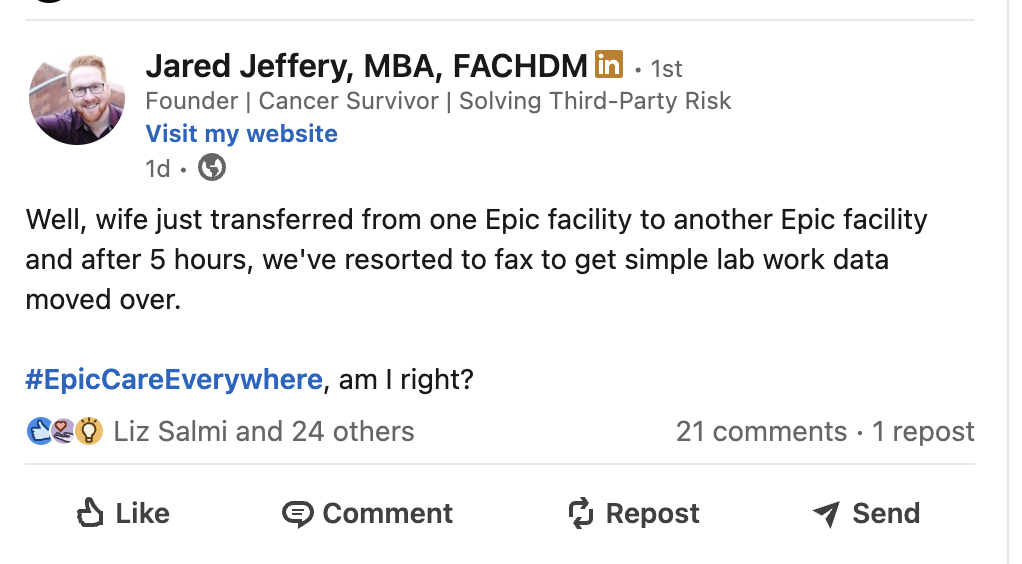
Can your staff actually access those exchange networks? Even when your organization participates in HIEs or TEFCA, many frontline nurses don’t know how to query them. If your staff can’t find information that’s technically “available,” it might as well not exist.
Does your portal meet current patient access requirements? Federal rules now require APIs that let patients move their data to apps they choose. Patients are already trying this access by connecting AI health assistants, personal health records, and care coordination tools. When your portal can’t support these connections, patients don’t always blame the app. They blame you:
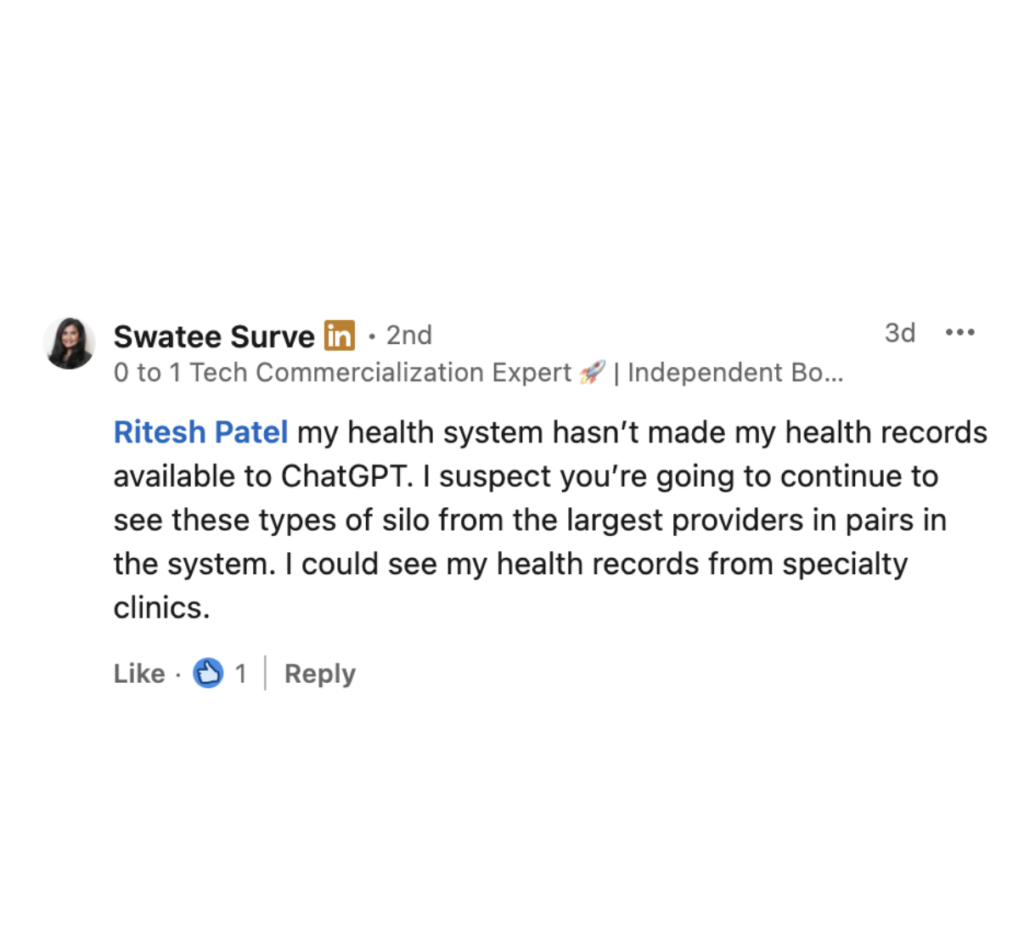
What are your EHR vendor’s priorities for FHIR updates? Some vendors are racing to implement new FHIR standards that prevent information blocking. Others are moving slowly. Rarely do organizations know which camp their vendor falls into, but patients feel the difference every time they try to share records.
Is your organization accidentally information blocking? Most people never do it intentionally. But when your policies require patients to come in person for records, your primary care to “flip it on” or charge fees for electronic access, or make them wait days for information that exists digitally…that’s information blocking, even if it’s wrapped in “privacy protection” language.
Most healthcare workers have no idea how to answer these questions. Most patients have even less idea what to ask.
But they’re all living with the consequences, one failed care transition at a time.
A Simple Transition Readiness Assessment
As Susan Clark shares on Converge Health’s blog, most organizations measure participation; few measure whether their investment actually fits into clinical workflows. Before your next all-staff meeting or town hall, try this usability check:
- The Password Test How many portals does a typical patient use across one episode of care?
- The Sharing Test Can a patient easily download and reuse their information? Have you tried it yourself?
- The Transition Test How does information follow patients between settings? (If the answer involves faxing or paperwork, friction exists.)
- The API Test Can patients connect third-party apps of their choosing?
- The Staff Burden Test How much staff time goes into helping patients retrieve or transfer data?
If coordination still relies on phone calls, PDFs, and that one staff member (you know the one) who has every fax number memorized, that’s not a failure.
It’s an infrastructure gap, and one we finally have the policy, APIs, and tools to close it!
Moving Forward Without Pointing Fingers
Here’s what matters: Nobody designed this system to be burdensome. We all built the best solutions we could with the tools (and budgets) available.
But somewhere between “checking the box” on patient portals and actually serving front-line staff and patients through transitions, we created something exhausting.
The first step isn’t buying new technology. It’s honestly assessing where the friction lives.
What Gets Measured Gets Improved
The questions in this post aren’t rhetorical. They reflect the core requirements of CMS’s Rural Health Transformation Program (RHTP) and the 21st Century Cures Act, requirements that focus on whether technology actually enables coordinated care, not just whether it exists.
The challenge: Rural communities are being courted by vendors promising “interoperability” and “technology innovation” without clear ways to measure if those investments will actually reduce burden, improve outcomes, or remain sustainable after grant funding ends. Every rural health technology investment must be evaluated not just on what it promises, but on what it measurably delivers.
What we’re developing: A framework to help rural health programs evaluate whether technology investments will genuinely serve their communities long-term, or leave them with expensive systems that don’t talk to each other five years from now.

We want to hear from you:
- Are vendors making promises about interoperability that you need help verifying?
- What metrics would actually prove technology is reducing coordination burden?
- How do you protect your community from solutions that work in demos but fail in real workflows?
Your insights will help us evolve this scoring tool to ensure it measures what matters most, so rural communities can learn from the hard-won lessons of urban health systems and large EHR implementations without repeating the same expensive mistakes. Smart rural health technology investment means you’ll be able to question vendors with specificity, show state leadership concrete evidence of improved care coordination, ensure your RHTP investments actually reduce staff burden instead of adding to it, and make investments that last beyond the grant cycle.
Because Mr. Rodriguez and his daughter shouldn’t need a PhD in health IT to participate in his care, and your staff shouldn’t spend hours hunting down, printing, faxing, and re-entering information that already exists.
Primary Record bridges disconnected health information systems, reducing the burden on patients, families, and frontline staff who shouldn’t have to manually move information that already exists. Learn more →